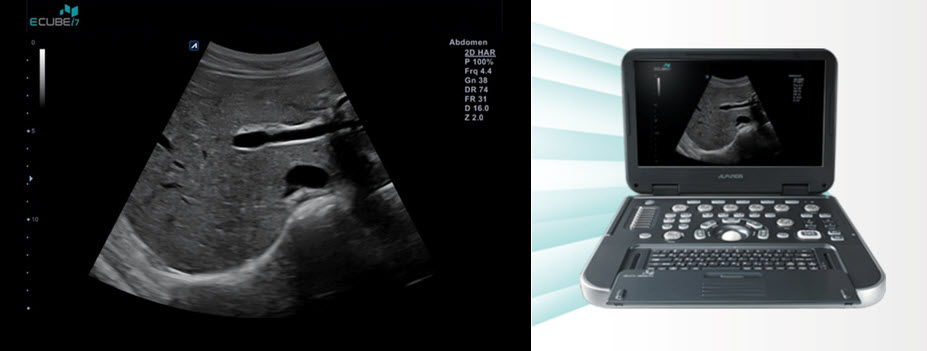
This week’s episode is with Dr. Carballido, an OB/GYN physician who is the medical director for the Alpinion ultrasound company. We discuss some great stuff about diagnostic ultrasound and what the future technology holds for us. Please join us for this week’s informative and entertaining discussion.

About Dr. Raphael Carballido [01:14]
- Raphael Carballido immigrated to the United States from Caracas, Venezuela
- He was able to practice in Venezuela for almost 25 years before coming to the United States
- He is the Medical Director for Alpinion which manufactures very high-grade ultrasound technology
- In this episode, we discuss:
- Elastography
- Different nuances of imaging with ultrasound for plantar fasciopathy
- Breast cancer
- Some of the developments with ultrasound imaging
He is an OB-GYN physician who loved the ultrasound since the first time he used it [05:14]
- He started doing breast ultrasound and incorporated breast imaging ultrasound in his practice, which is not very common for the OBGYN.
- He says that when you find a tumor by palpation, usually that's too late.
- A tumor that will be between two to three centimeters in diameter will be a stage two or three.
- That means mastectomy, chemotherapy, radiotherapy, or many other things.
- When you put the ultrasound on top of the spot where the MRI says there is suspicious lesion, we were able to see it clear.
Ultrasound is able to see cancer in the breasts when it's under 10 millimeters. [05:42]
- Dense breast mammography has limitations to see the cancer that is hidden inside that dense breast tissue.
- In the United States, almost 50% of population has dense breasts. The chances of having breast cancer for a woman is one out of eight.
- In China, 70 to 80% of the population have dense breasts. The chances are one out of six, they have a higher incidence.
- It is influenced with hormones.
- If you're using hormones, you can you can keep the breast dense for many years after the menopause. That is also a risk factor.
- in the last three years, we haven't been able to change the number of deaths by breast cancer in the world.
- In the United States, we have 42,000 deaths by breast cancer every year
- That is the number one killer for cancer in women.
- As far as a breast ultrasound screening method, they use mammogram which sometimes miss cancers.
- The path that some doctors are taking if mammogram misses cancers is to do MRI. MRI, as an imaging modality is excellent and very sensitive.
- For doing MRI, you need to inject gadolinium contrast. It can have secondary effects in your brain or your kidneys.
- You need to have another option different to MRI. Using MRI as a screening method for breast cancer is an error.
Dr. Carballido began to work as a medical director for a company dedicated only to ultrasound. [11:56]
- One of their major applications is everything related to MSK and breast imaging with a high frequency transducer.
- He had the chance to meet a genius radiologist in California, Dr. Kevin Kelly:
- He also found that mammogram was not good enough to find cancers
- He invented a robotic arm to do breast ultrasound screening and was successful.
- Cancers on their 10 millimeters is a threshold that we want to use because that means stage 1
- Stage one in breast cancer means that your chances are almost 100% of being cured.
- Kelly invented this machine but it got rejected because it didn't have a CPT code to be reimbursed.
- It also takes a bit longer to read than an MRI or handheld ultrasound.
The problem with handheld ultrasound is that it is very difficult for the human eye to see a four-millimeter cancer in the breast. [14:26]
- Doing handheld ultrasound screening requires a lot of experience.
- The automated breast ultrasound machine was a real solution.
- Carballido is currently working actively working with this company in developing the new generation of these machines.
- The robotic arm is now completely automated.
- Using artificial intelligence to find the cancer
- The machine can actually incorporate 3D Ultrasound Power Doppler to see their vascularity which is very important for breast cancer
- Elastography which is also very important to distinguish between malignant tumor versus benign.
All of us have someone that we know that has gone through this process of finding breast cancer treatment. [16:54]
- Once someone goes to stage two or three, they need to go to mastectomy, radiotherapy, chemotherapy, and the stress for the family and the patient.
Thermography has been relegated in the United States as some type of pseudo imaging. [18:28]
- Although there are some countries that use a lot of thermography
- Similar to this early prototype that Dr. Kelly developed.
- It's a lot of pushback to it because there isn't a CPT code.
- It possibly steps on the traditional toes of Radiology
- MRIs are more profitable
- In the future, the normal mammogram will not exist.
- How many millisieverts of radiation exposure is there with a mammogram?
- We're irradiating these folks every year that could be potentially injurious in itself.
- The machines have been improving their amount of radiation to the point where it's low.
The main reason why we don't do ultrasound mammography for years is so we don't send radiation to that press which can cause cancer in the future. [20:52]
- Mammography is very limited when you have dense breasts.
- When you're in your 30s, then the breast is dense. After you're 40 or 45, it tends to be fierier and so is the consistency of the tissue changes.
“With ultrasound, which we've already discovered in the lower extremity, is very inexpensive, portable, dynamic, and has all of these advantages to an MRI.”
- It’s at the point of examination versus wanting to image this.
- I have to write an order have to get them scheduled for an MRI in 30 seconds
- I can have that transducer on them in the office and I'm seeing something very real.
- If this technology was really accepted, you could start instituting screening with this when a young lady's 20 and get a baseline.
- If there's something questionable, then that that patient would need to be serially scheduled more frequently.
- This can be a machine that can be in the clinic setting.
- One thing a woman does is going to their annual checkup for the Pap smear.
- The pap smear has the same objective—to find that the cancer treatments are the pre- cancer stage.
- The same thing happens with gastric cancer which was a big issue in the public health system in Japan.
- They invented the endoscopes because when they could see the cancer when it was small, it could be easily treated and the outcome will be very good.
- By law, they need to have gastroscopy and colonoscopy done every year.
- It's a lot less expensive to pay for a gastroscopy than to put somebody in for full blown gastric or stomach cancer
- If insurance companies make the numbers—treatment of breast cancer in an advanced stage in one patient is the same amount when paying 1000s of screenings.
All of the sponsors of this podcast are listed at podofinquiry.com. [25:33]
- You can get great offers on these fantastic products and services.
- Their portable iCube 7 retails for $21,000. But you can get it discounted at most medical meetings for $19,000. But my listeners will get it discounted to $15,900.
- Use code SBPOI to take advantage of this incredible offer.
When you can implement musculoskeletal ultrasound imaging you first know exactly what you're dealing with. [27:14]
- Using the example of plantar fasciopathy, people were coming in with heel pain and they were treated by cookie cutter algorithms.
- Many times, once examining these patients with high resolution diagnostic ultrasound, they'd have a pristine plantar fascia, but yet they had been given the diagnosis of plantar fasciitis at that time.
- They were being treated for something that they really didn't have, which was expensive for them and their insurance company.
“Accurate diagnosis really leads to more optimal treatment.”
Why is there such a hurdle to getting people to adopt diagnostic or MSK ultrasound? [29:03]
- The major hurdle is training.
- They see it in a theory, but they don't use it.
- They were trained only to use X-ray which is much more expensive.
- The lack of interest of the doctors of the podiatrist to use ultrasound because they don't see the need for using it.
- They don't realize that actually is more than a CPT code.
- They don’t realize that when you're using ultrasound in podiatry, you can actually see in real time what is happening in a moment.
- You can move it; you can put pressure.
- You can see what happens with the fluids in there, you can see the tendons moving.
- It's real time assessment of what is happening.
- They don't realize that it's not difficult to learn how to ultrasound for basic podiatry.
- They don’t realize that once you begin to use it, it becomes an extension of yourself.
- It’s like a part of your clinical examination, it's something that you need to use for every case.
- When it comes to do the injections, you might think that you're doing right injecting blind but the accuracy of blind injection is about 30% yet for plantar fascia.
This study with 18 cadavers was never published. [33:53]
- The goal was with methylene blue in the syringe and injected only to the plantar fascia without any guidance.
- It was only 6 out of the 18 or about 30%.
- The same thing happens in other areas of MSK where they do blind injections.
- They actually work when the biological medication they're using is injected in the right place.
- Carballido participated in a workshop where doctors with experience were trying to inject the suprascapular blindly.
- Once they put the ultrasound system on top of the needle, the needle was completely out of the target.
- The amount of fluid that they inject is important because if you inject more than needed, you will actually disrupt more fibers or tissue than needed.
“With an ultrasound, you can see in real time how much you need to inject according to the size of the lesion.”
- Ultrasound serves like a method to follow up in the progression of what you're doing with that with the patient.
Many publications have now ultrasound as the gold standard for shoulder assessment. [37:23]
- The main reason is it is real time, low cost, and you can evaluate the function.
- You don't see the rotator cuff move on an MRI.
- Plantar plate ruptures of the lesser metatarsophalangeal joints are extremely common, but are rarely picked up on an MRI.
- When they're in the tube, there's no stress on that metatarsophalangeal joint.
- In the clinic after they had this “normal MRI”, and you do a dynamic examination, you can see the plantar plate just open up.
“Real-time dynamic examination trumps static MRIs. Ultrasound MSK is the gold standard.” [38:59]
- For plantar fasciopathy, we're able to evaluate what's really going on with ultrasound such as the compressibility of their fat pad. These can't be assessed by MRI.
- When doing an ultrasound guided placement of something like BPC 157, amnio, or PRP, you can see on ultrasound that just fill up the plantar fascia.
- It's beautiful to see that you're in the right spot because you are using ultrasound guidance, and then you put that fluid in there.
- It's experiential and you see things that you didn't see before, because you're looking more for them.
- When the patient sees this biologic that you're putting disseminate all through that area starts the healing process because there's a mind-body connection.
- There's benefits not only for the practitioner, but also for the psychology of the patient.
- It validates them because it confirms with them that they have real pathology.
“Financing is not the real issue, it's training.” [44:00]
- Pain management doctors were trained to use X-ray, so they expose themselves and the patients every day to high radiation.
- They’re in front of the machine injecting to treat the pain in many parts of the body under X-ray guidance with a CRM
- In other countries, they use ultrasound which has the same results as a CRM but is faster, better, accurate, and without radiation.
- When Barrett finally made the leap to putting an ultrasound into the clinic, one of the sonographers came down and spent a day with him.
- Having somebody just looking over your shoulder that can point out really accelerates your learning curve.
- Then the next step after is that you just have to keep doing it.
- As you continue to do it, your experiential body builds up on what to look for.
- In the lower extremity, the plantar fascia is one of the easiest things to do from an ultrasound standpoint.
Now, better visualization tools in ultrasound machines have been incorporated. [47:20]
- You can tell for sure where the tip of the needle is if you allow for infiltrate flow.
- When you're injecting, you can see the fluid actually grinding out of the needle and filling in that space.
- One of the problems with echogenic needles is that the smallest gauge needle that you can get is 25 gauge.
- You can see a 30-gauge needle on the ultrasound and long axis if you know what you're looking for.
- When doing an ultrasound-guided radiofrequency ablation, the tip of the radiofrequency needle starts to heat up and you can actually see those changes visually.
- You can see the bubbles because they're right inside the fluid.
- Once you build up your experience level, they're very easy to see.
“Do it every day with every patient that will give you a baseline to know what you're supposed to see.”
- You can see normal things in patients that have abnormal tissue or abnormal pathology by looking at different areas as well.
One important thing is how ultrasound systems have been evolving and getting better over the time. [51:39]
- Now we can reach higher frequencies that we couldn't reach before.
- We have expanded the bandwidth of the transducer.
- Before you go from 5 to 10 megahertz, then 3 to 12.
- Now, we have pros that can go from 3 to 19, or 10 to 25.
- With a 10 to 25, you will have a limitation of penetration.
- The higher the frequency, the lower the penetration
- For nerves that are small and close to the skin, you will be able to see them in a way never before.
How Ultrasound works. [53:31]
- When we train the doctors, we train them to move the transducer from one side to the other to make a fan movement.
- Structures like tendons and nerves turn corners, so you have to be able to bring your transducer.
- The way ultrasound works is that it shoots out a sound wave and then it comes back to the transducer as it bounces.
- If I was going to throw a tennis ball against the wall, and I wanted it to come back to me, I would be perpendicular to that wall.
- If I went on an angle and threw the ball to the side, it's going to bounce off to the other and that's going to give a hypoechoic signal.
- You can interpret it as a lesion, but it's not.
- To see it better, you cause anisotropy to erase the tendons and keep the nerve.
Elastography has been in the ultrasound industry for many years. [55:40]
- We are currently using ultrasound elastography for liver disease for taking the different stages of fatty liver fibrosis and cirrhosis.
- It is very accurate and has a CPT code that has been widely accepted.
- Hurdles with elastography:
- Before we were using something called strain elastography lithography which was very subjective.
- 3D results were not very reliable or reproducible.
- We're using a new type of elastography
- It gives you a very accurate number measuring kilopascal
- This tells you about the elasticity and stiffness of the tissue
- It can give you the number in 1.5 seconds: you set the point and it gives you a number, and after repeating it 12 times, it gives you the median. The median will take out those values that are very out of range. The higher range will give you a confidence interval.
- You can trust the result. It is very reliable and reproducible.
- It doesn't matter if other technician does it next week, we'll get the same results.
- The same thing is being used for breast imaging, for distinguishing malignant tumors from the benign tumors.
- The new trend now is to use MSK ultrasound.
- One of the first uses for it is muscle tears, especially in athletes where people really need that muscle to be healed completely.
Shear wave elastography gives you a very accurate number of what the lesion is. [59:00]
- You can also see it in color and the dimension of the tear
- Then you apply your biologics of whatever you're going to use for treatment.
- You can see the outcome of that treatment over time.
- It takes some of the clinical guesswork out by the sports medicine physicians to say an athlete is ready to go back.
- You want to put them back to play again soon as possible, but you can create more damage.
“With ultrasound, you can have a very accurate way to say when that muscle has the same structure and strength as the rest of the other tissues around it.”
When Dr. Barrett implemented ultrasound into the practice [1:00:23]
- He was playing around with the color flow one day and was just hitting the transducer on this very diseased plantar fascia
- It would light up all around except in the area that was really degenerative
- He went to the other side and would see a more consistent signal through the tissue.
- It was like one of those weather radar maps where you see your city and all the bad clouds around it.
- He was using PRP and then look at the patient in 8 or 10 weeks
- After their infiltration in that area around the city, there were no clouds.
- The good thing now is that because you have this grading scale for the tendinopathy
1:02:29
- Those machines are a little bit more expensive than the ones that you can use in regular practice.
- It may be worth it for certain practices where they deal with athletes or people who they need to have that added layer of technology.
- The Alpinion machines are incredible compared to other machines that cost the same that don't do nearly what the Alpinion machines do.
Alpinion has a philosophy of providing extreme value. 1:05:00
- They want to be sure that whatever they provide will give clinical significance and at a good value.
- What they’re trying to do is to incorporate the training part to the sales process.
“It’s hard to practice without ultrasound if you really want to deliver the highest level of care.”
- These folks that claim they're experts in heel pain and they don't need an ultrasound, because their thumb is just good when it presses on the medial calcaneal tubercle, are like guys claiming to be an astronomer but don’t believe in telescopes.
- There's no way you can lose by putting this in just by increasing the quality of your care.
- They still do pay you for ultrasounds because there are CPT codes.
- Of all the technology out there, musculoskeletal ultrasound/sonography is probably one of the best returns on investment.
People always say you don't really need an ultrasound for taking care of a plantar fascia problem. 1:08:20
- And the answer is if I was going to invite you to go out hunting tomorrow, don’t you want to know if we're going elephant hunting or mouse hunting?
- Because we might take a different gun for the mouse than we would for the elephant.
- With plantar fascia, within 30 seconds, you know whether or not you have a disease and its severity.
- Is this going to respond to some stretching and orthotics
- Is this going to be something that needs more intervention, like peptides, amnio, or stem cells?
- You're not going to treat the mouse the same as you're going to treat the elephant.
- It's just so powerful for patients because they can come in, and get a definitive diagnosis of plantar fasciopathy and its extent.
- You can deliver that care more timely, which gets them back to their regular day-to-day quicker and which saves them money.
Education is Power. [1:10:48]
- If you know more things, you're able to treat more things and able to reach a different subset of the population.
- It's just going to expand the value of your practice exponentially.
How can I learn about all this cool stuff that I hear on the Pod of Inquiry? [1:12:56]
- Dive in with an intensive hands-on experience at our educational courses.
- People have been asking about peptides, hydrodissections, diagnostic ultrasound-guided nerve blocks, and management of complex heel pain to mention just a few.
- The Pod of inquiry and US Neuropathy Centers are happy to announce that we will be hosting several instructional courses that you can now register for.
- Our first two courses will be held on April 1 and April 2, 2023 in our facility at Marietta, Georgia.
- On Saturday, we will be holding an intensive day of diagnostic ultrasound imaging, interpretation, and interventions.
- On Sunday, April 2, 2023, Heel Pain boot camp returns. This is version 3.0.
- The heel pain boot camp was first launched about 10 years ago and it was wildly successful and this one will be more of the same.
- We will get into a deep dive into all things peptides: Peptides like BPC 157 and thymosin beta 4.
- I can assure you of the ultimate learning experience and that you can get your practice into the future by signing up now.
- You can register for them by clicking here.
Alpinion Medical Systems
The deal: USE CODE: SBPOI
The portable i7 retails for $21k, you can usually get it discounted to $19k at a medical meeting, but my listeners will get it discounted to $15,900. This has never been offered anywhere for a new portable system with the engine of console system use code SBPOI and take advantage of this incredible offer. You would pay probably twice this with other companies to get the same level of technology.