Show Notes
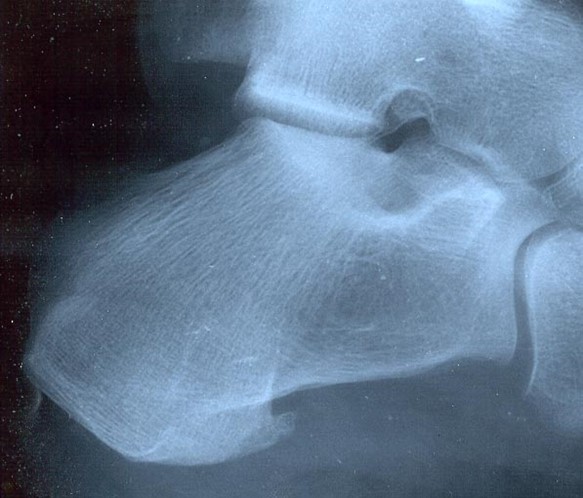
Dr. Stephen Barrett 01:08 Is it an elephant? Or is it a mouse?
Dr. Stephen Barrett 03:10 Anatomical delineations (Zones) of the plantar fascia for diagnostic sonography.
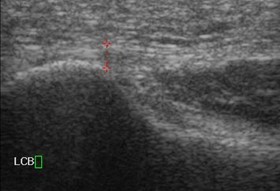
The normative study to determine dimensions of the plantar fascia with ultrasound imaging. LINK (page 221).
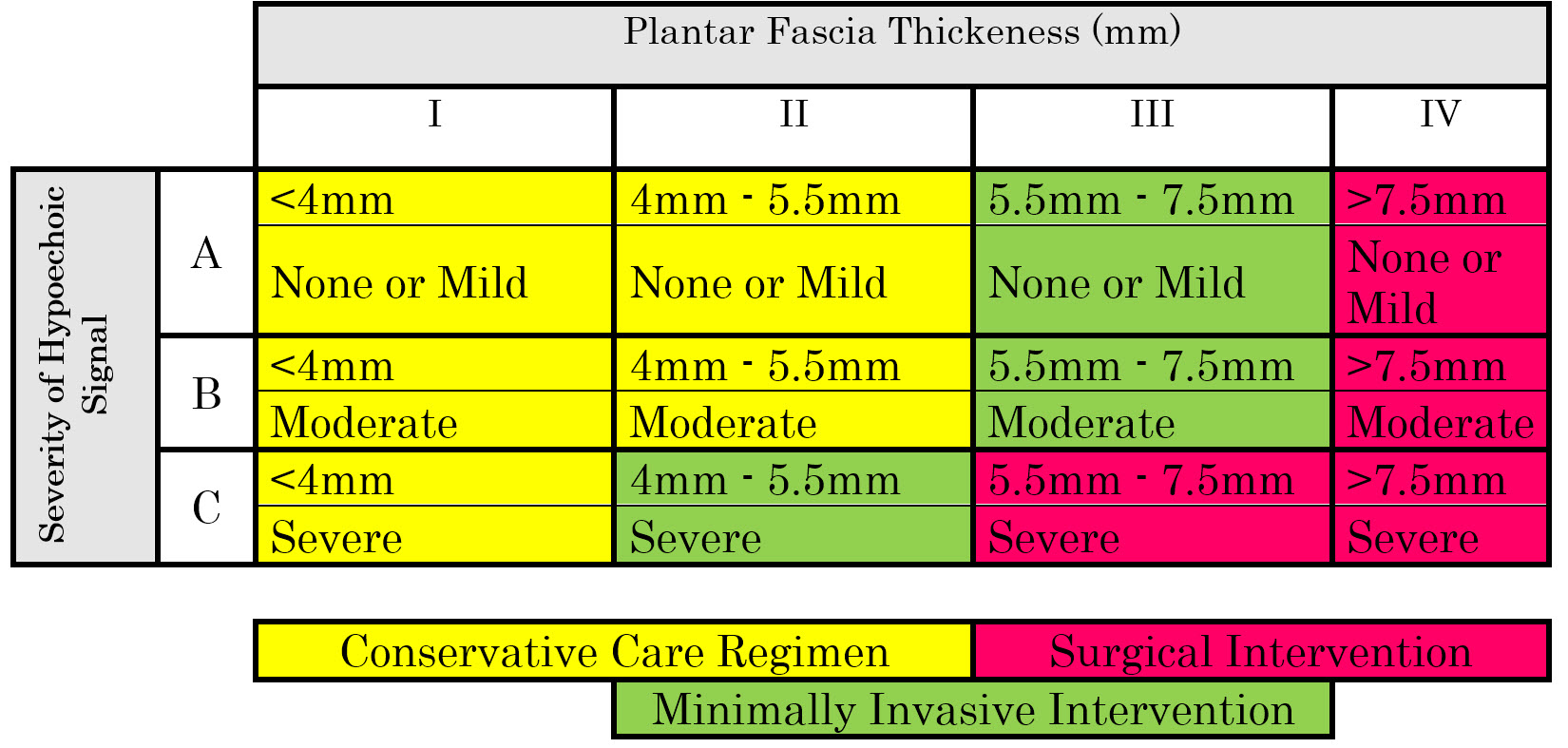
Discussion of the different zones of the plantar fascia and their normatives.
Dr. DuCasse and Dr. Barrett 09:13 How does a zone “C” abnormality subordinate the other findings?
Dr. DuCasse 12:23 Evaluation of other soft tissues in the heel with sonography.
Dr. Barrett 12:31 Fat pad, anisotropy, hyper or hypoechoic? Initial clinical experience with PRP, Amniotic fluid, and BPC-157.
Dr. DuCasse 17:47 The heel pain questionnaire. LINK (p. 218)
Dr. Barrett 18:13 Nuances of the MEHPS questionnaire.
Dr. Barrett 19:52 What does staging and grading really do? Baxter’s nerve?
Dr. Barrett 20:18 Nonsensical nomenclature. “Baxter’s Nerve” It was Roegholt in 1940 LINK
Dr. DuCasse 21:37 The Chicken or the Egg? Multiple etiology heel pain.
Dr. Barrett 22:09 The debate in Chicago. Biomechanical sequelae of EPF. Li and Muehlman study LINK
Dr. Barrett 27:27 Less morbidity with EPF
Dr. Barrett 31:21 The pristine plantar fascia—now what? Can heel pain be the 1st marker of type II DM?
Dr. DuCasse and Dr. Barrett 33:25 Symptom treaters. What about Equinus?
Yeah. How do you How did you figure that out? Yeah. Well,
Dr. DuCasse 34:55 Her experience in residency treating heel pain.
Dr. Barrett 36:26 What is the barrier to entry for implementation of DUS in the podiatric practice?
Dr. DuCasse 36:36 Ultrasound guidance for injection therapy for plantar fasciitis.
Dr. Barrett 38:44 Describes how he implemented DUS in his practice and the learning curve associated with this technology.
Dr. DuCasse 41:59
I mean, even even utilizing the ultrasound in the office. Right, right. Doesn’t cost you anything. But the ultrasound on the patient? No, I mean, maybe a little time. Yeah. And just, you know, a couple pennies worth of gel really, right. But the value that you gained from seeing the actual tissue that you’re treating and improving that patient’s quality of life, even if you’re not billing for it, you’re you’re a better clinician, because you’ve seen what you’re doing
Stephen Barrett 42:25
right. Now, if they said, we’re not paying for ultrasound anymore tomorrow, which insurance companies could do because they do that with other stuff? Or they could do it? They would, it wouldn’t change my utilization of ultrasound whatsoever. Because I, I just think it’s it’s also a really good metric for the patient. Because the patient’s can look at that. And they can look at their other heel. And they know
Dr. DuCasse and Dr. Barrett 42:50 The power of ultrasonography for the practitioner and the patient. Regenerative therapy.
Dr. DuCasse 44:30
no, but I think the point of it is that we could be doing a lot better job at treating a few of these patients a little more than a few of these patients. And if we have the training, and if there are resources out there that can help us to do that we should utilize them, right. If you don’t know you don’t know. Right? Right. Right. But if you do know and you don’t do that’s a different thing, right.
Stephen Barrett 44:53
And the thing too, is that the eyes can’t see what the mind doesn’t know. And once the He’s, once these guys come through these courses, and they know what to look for. Suddenly they’re all there. Yeah, they were never there before. That’s date. They are all there is very, we just went spelunking.